Get Free Delivery With No Minimum Order
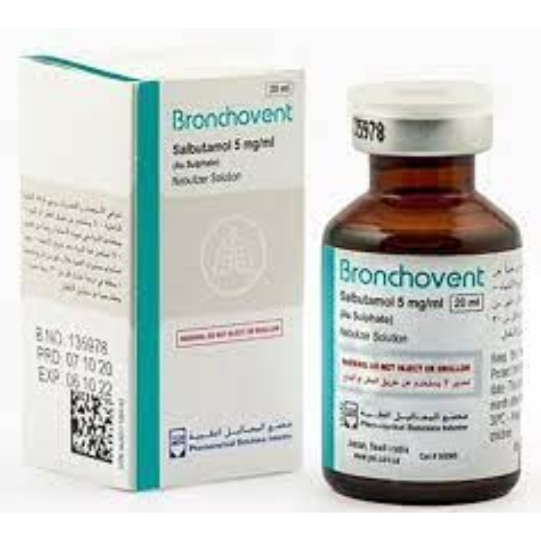
BRONCHOVENT 5/MG NEBULIZER SOLUTION 20ML
- Sku : I-030845
Key features
BRONCHOVENT 5 mg/ml nebuliser solution contains the active ingredient salbutamol. It is a selective short-acting beta-2 adrenergic agonist that activates adenylate cyclase, increases intracellular cAMP and relaxes bronchial smooth muscle to produce bronchodilation. It is indicated for the treatment and prevention of bronchospasm in patients with reversible obstructive airway disease, including asthma and chronic obstructive pulmonary disease (COPD). Available by prescription as a 5 mg/ml nebuliser solution in a 20 ml pack.- Brand: BRONCHOVENT
- Active Ingredient: SALBUTAMOL
- Strength: 5mg/ml
- Dosage Form: Nebuliser solution
- Pack Size: 20 ml
- Route: Inhalation use
- Prescription Status: Prescription
- Therapeutic Class: Respiratory
- Pharmacological Group: Beta-2 Agonists
- Drug Class: Short-Acting Beta-2 Adrenergic Agonist (SABA)
- Manufacturer: Pharmaceutical Solution Industries (PSI)
- Country of Origin: Saudi Arabia
- SFDA Registration No.: 1108222472
- Shelf Life: 24 months
- Storage: store below 30°c
- Symptom Target: Bronchospasm, wheezing, shortness of breath
- Sedating: No
Indications
Approved Uses
Treatment and prevention of bronchospasm in patients with reversible obstructive airway disease, including asthma and chronic obstructive pulmonary disease (COPD).
Off-Label Uses
Adjunct treatment of acute hyperkalemia (typically via inhaled/nebulized beta-2 agonist as part of emergency management).
Dosage & Administration
Dosing by Condition
Acute bronchospasm (asthma/COPD) via nebulizer: Adults and adolescents ≥12 years: 2.5 mg (0.5 mL of 5 mg/mL) diluted to 3 mL with sterile normal saline, 3-4 times daily; Children 2-12 years: 0.1-0.15 mg/kg/dose (max 2.5 mg) 3-4 times daily.
Initial Dose
2.5mg (0.5ml of 5mg/ml solution) diluted with normal saline, nebulised
Maintenance Dose
2.5 mg to 5 mg via nebulizer every 4 to 6 hours as needed.
Maximum Dose
Adults: typically 2.5-5 mg per nebulised dose up to 4 times daily (usual max 20 mg/day); higher doses (up to ~40 mg/day) may be used only in severe acute asthma under close medical supervision/monitoring.
Children's Dosage
Children 2-12 years: Initial 0.1-0.15 mg/kg/dose (approx 1.25-2.5 mg), not to exceed 2.5 mg 3-4 times daily by nebulization; <2 years: 0.2-0.6 mg/kg/day divided every 4-6 hours (use under specialist supervision).
Dose Adjustment Notes
Use the lowest effective dose; frequent need indicates poor control and requires reassessment; use caution in cardiovascular disease/arrhythmias, hyperthyroidism, and diabetes, and consider closer monitoring/starting lower in patients more sensitive to beta-agonist effects; monitor potassium (and glucose in diabetics) with high-dose or frequent use.
How to Take
For inhalation via a nebulizer (typically jet nebulizer) only; measure the prescribed dose and dilute with sterile 0.9% sodium chloride to an appropriate nebulizer fill volume (commonly ~2-4 mL per device instructions), then inhale the mist through a mouthpiece or mask until the nebulizer sputters/stops; do not swallow or inject; do not mix with other medicines in the nebulizer unless specifically directed.
How to Prepare
Measure the prescribed dose from the 5 mg/mL solution and dilute with sterile 0.9% sodium chloride to a nebulizer fill volume typically 2-4 mL (commonly ~2.5-3 mL); administer immediately and discard any unused prepared solution.
Side Effects
Common Side Effects
Tremor/shakiness, palpitations, tachycardia, headache, muscle cramps; hypokalemia can occur especially with high doses/frequent nebulization.
Side Effect Frequency
Common: tremor, headache, tachycardia/palpitations, muscle cramps; hypokalemia is a known dose-related effect that is typically listed as common/uncommon (not rare), while arrhythmias and paradoxical bronchospasm are rare.
Safety & Warnings
Contraindications
Hypersensitivity to albuterol or any component of the formulation.
Warnings & Precautions
Caution in cardiovascular disease/arrhythmias, hypertension, hyperthyroidism, diabetes, and in patients prone to hypokalemia; monitor potassium in severe asthma/high doses; stop immediately if paradoxical bronchospasm occurs; increasing SABA use signals worsening control and need for controller therapy review (not a substitute for inhaled corticosteroids in persistent asthma).
Age Restriction
No absolute minimum age; nebulised salbutamol can be used in infants and children, with dosing based on age/weight and clinical response under medical supervision (especially in infants).
Drug Interactions
Drug Interactions
Non-selective beta-blockers (e.g., propranolol) antagonize effect/bronchospasm risk; other sympathomimetics add CV effects; diuretics and xanthines (e.g., theophylline) increase hypokalemia risk; digoxin toxicity/arrhythmia risk may increase via hypokalemia; MAOIs/TCAs may potentiate cardiovascular effects.
Interaction Severity
MAJOR: Non-selective beta-blockers (e.g., propranolol) can antagonize bronchodilation and precipitate bronchospasm; MODERATE: Diuretics, systemic corticosteroids, and xanthines (e.g., theophylline) increase hypokalemia risk; TCAs/MAOIs may potentiate cardiovascular effects; digoxin-beta-agonist-induced hypokalemia may increase arrhythmia risk and lower digoxin levels.
Food Interaction
No restriction.
Special Populations
Pregnancy
Caution
Breastfeeding
Caution
Children
Children 2-12 years: Initial 0.1-0.15 mg/kg/dose (approx 1.25-2.5 mg), not to exceed 2.5 mg 3-4 times daily by nebulization; <2 years: 0.2-0.6 mg/kg/day divided every 4-6 hours (use under specialist supervision).
Kidney Impairment
No routine renal dose adjustment for inhaled/nebulised salbutamol; use clinical monitoring in severe renal impairment if high/frequent doses are required.
Liver Impairment
No adjustment needed.
Storage & Patient Advice
Preparation Instructions
Measure the prescribed dose from the 5 mg/mL solution and dilute with sterile 0.9% sodium chloride to a nebulizer fill volume typically 2-4 mL (commonly ~2.5-3 mL); administer immediately and discard any unused prepared solution.
Stopping the Medicine
May be stopped without taper; do not rely on frequent use-seek medical review if needing it more often or if symptoms worsen.
Overdose
Symptoms: tachycardia/palpitations, tremor, agitation, hypokalemia, hyperglycemia, lactic/metabolic acidosis, nausea/vomiting; severe: arrhythmias/ischemia and rarely seizures. Management: stop drug, supportive care, ECG and potassium/glucose monitoring and correction; consider a cardioselective beta-blocker cautiously for severe cardiovascular toxicity.
Patient Counseling
Rescue medicine for quick relief: use only by nebulizer for inhalation as prescribed; measure the dose accurately and dilute with normal saline to the nebulizer’s required volume; do not swallow or inject; if you need it more often than prescribed or it becomes less effective, seek medical review (poor control); expect possible tremor or fast heartbeat-seek urgent care for chest pain, severe palpitations, or worsening breathing; clean the nebulizer as instructed; store below 30°C.
Monitoring Requirements
Monitor symptom relief/need for repeat dosing and lung function (PEF/FEV1) when applicable; during high-dose/frequent nebulization monitor heart rate and blood pressure, and check serum potassium; monitor blood glucose in patients with diabetes or when using high doses.
Pharmacology
Mechanism of Action
Selective short-acting beta-2 adrenergic agonist that activates adenylate cyclase, increases intracellular cAMP, and relaxes bronchial smooth muscle to produce bronchodilation.
Onset of Action
Typically within about 5 minutes (often 3-5 minutes) after inhalation/nebulization, with peak effect around 30-60 minutes.
Duration of Effect
Approximately 3-6 hours.
Half-Life
Elimination half-life 5-6 hours after oral administration; plasma levels peak at 0.5 hours after nebulized dose.
Bioavailability
Systemic bioavailability after inhalation is limited; roughly ~10-20% of the inhaled dose reaches the lungs with the remainder swallowed, and systemic absorption occurs from both pulmonary and gastrointestinal routes (overall systemic exposure is generally low at usual inhaled doses).
Metabolism
Limited hepatic/extrahepatic metabolism mainly by conjugation to an inactive sulfate (salbutamol 4′-O-sulfate).
Excretion
Primarily renal: most of an absorbed dose is excreted in urine within 24 hours as unchanged salbutamol and as the inactive sulfate conjugate (commonly cited ~70% in urine; remainder mainly in feces).
Protein Binding
Low protein binding, about 10%.
Product Information
Available Dosage Forms
Nebuliser solution, metered-dose inhaler, dry powder inhaler, oral syrup, oral tablet, intravenous injection.
Composition per Dose
Each 1ml: 5mg salbutamol (as salbutamol sulfate)
Generic Availability
Yes
OTC Alternatives
No OTC alternative for nebulized salbutamol; this product is prescription-only per SFDA legal status.
Symptom Target
Bronchospasm, wheezing, shortness of breath
Sedating
No
Legal Disclaimer - Al Mujtama Pharmacy
The product information provided is derived from verified pharmaceutical references and is intended for general health education only. It is not a substitute for professional medical advice, diagnosis, or treatment.
Al Mujtama Pharmacy assumes no legal or medical liability for:
- Any therapeutic decision made based on the information displayed without consulting a licensed physician or pharmacist
- Any discrepancy between the information provided and the product's package insert or SFDA guidelines
- Any misuse of medication resulting from personal interpretation of the content displayed
Important notice: Drug formulations and instructions may vary between production batches. Always rely on the leaflet included inside the product packaging you have, and consult your pharmacist or physician before starting, adjusting, or discontinuing any medication.
By using this content, you acknowledge that you have read this disclaimer and agree that Al Mujtama Pharmacy bears no liability arising from reliance on this information as a substitute for direct medical consultation.
Your health is a trust - always consult your doctor first.
-1744229570.gif)